sb4
Senior Member
- Messages
- 1,916
- Location
- United Kingdom
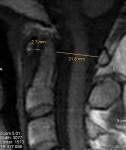
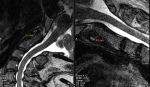
@Hip Very interesting, thank you. I hear you on the low CCI symptoms, that combined with no response to traction is quite significant in terms of thinking it is not this. However I do have some symptoms which make me think maybe, my neck is quite (uncomfortable?) at night time in most sleeping positions. I have weird yet slight neck ache and back ache that appears in the evening and coincides with the time of day I feel best. Perhaps that is from disc bulges as it feels in a similar place (lower neck). Then there is the TMJ, receded gums, EDS in imediate family, and now, what seems to be significantly past the norm neck extension, even though P Smith thinks this isn't causing issues.
@pattismith I have not measured translational BAI, could you give me a quick run down on what it is and I will look at it tomorrow morning.
@pattismith I have not measured translational BAI, could you give me a quick run down on what it is and I will look at it tomorrow morning.