Chap. 7 Contin. Unhelpful thoughts and alternatives (!)
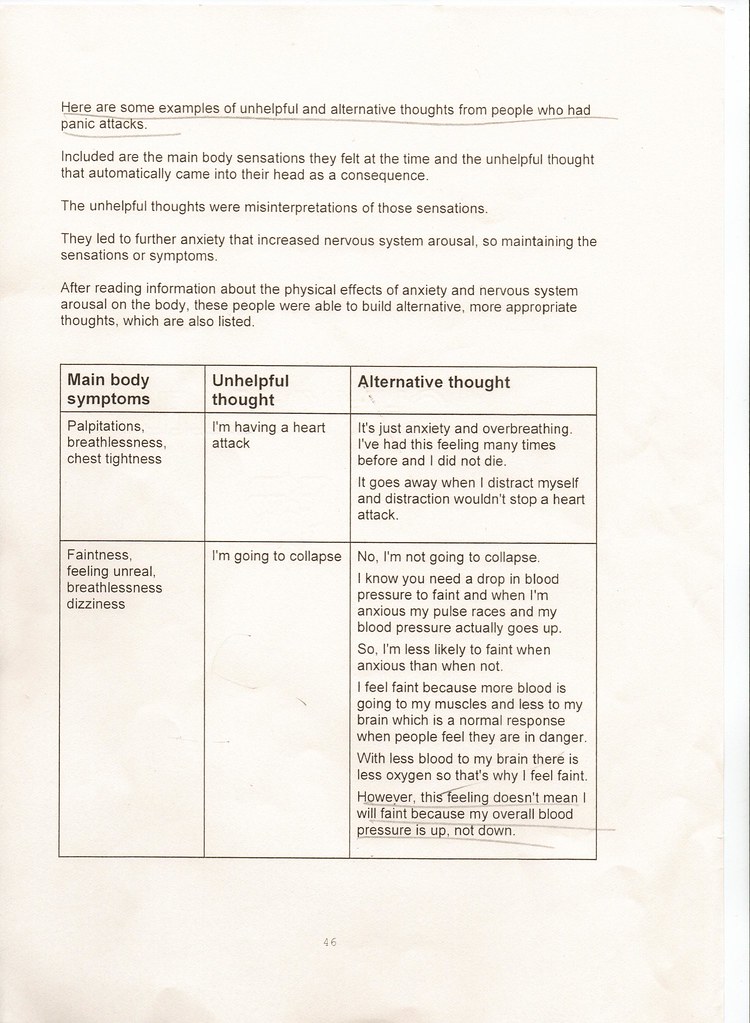
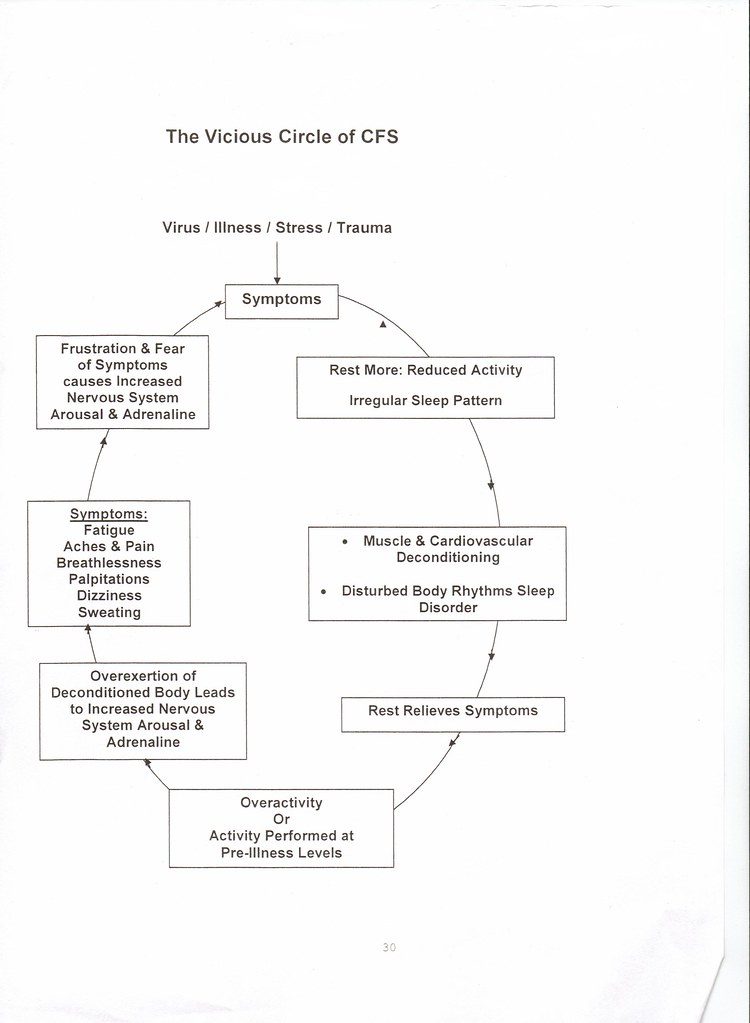
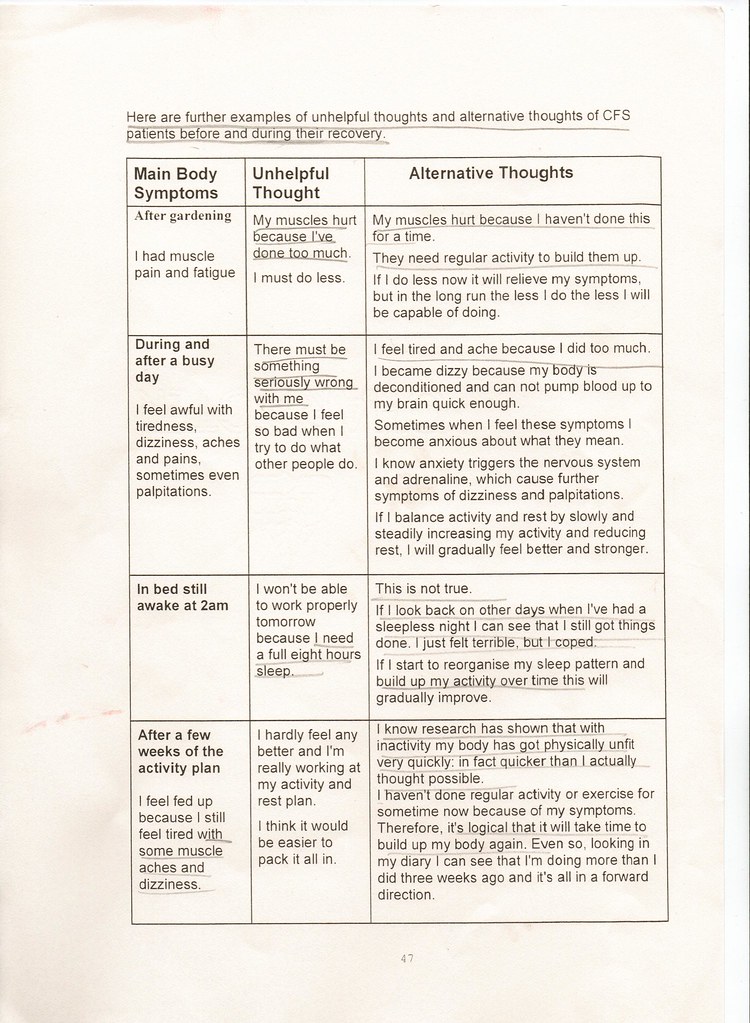
I have scanned in pages 46-48, and put them below. They have boxes for Symptoms, Unhelpful Thoughts and Alternative Thoughts, which are worth reading just for a laugh (again some things underlined by me).
They keep banging on about building up activity in their "Alternative" (i.e. helpful/"correct") thoughts section. So whatever symptoms you have, GET is the answer.
I will quote some of this stuff here to give idea as to the stupidity of some of their ideas.
Main body symptoms
Faintness, feeling unreal, breathlessness dizziness
Unhelpful thought
I'm going to collapse
Alternative thought
No, I'm not going to collapse.
I know you need a drop in blood pressure to faint and when I'm anxious my pulse racces and my blood pressure actually goes up.
...ths feeling doesn't mean I will faint because my overall blood pressure is up, not down
[Orla - of course many people with ME/CFS will have low, or unstable blood pressure, on standing, and possibly other (organic) problems to do with standing, so it is not unhelpful of them to interpret their symptoms as a problem and to sit down.]
Main Body Symptoms
After gardening
I had muscle pain and fatigue
Unhelpful thought
My muscles hurt because I've done too much
I must do less
Alternative thoughts
My muscles hurt because I haven't done this for a time
They need regular activity to build them up
[Orla - they see symptoms as a sign of deconditioning not disease, and because of this they are giving appalling advice here]
Main Body symptoms
During and after a busy day
I feel awful....
Unhelpful thought
There must be something seriouly wrong with me....
Alternative thought
I feel tired and ache because I did too much
[Orla - didn't they just tell us a minute ago that this last thought was an unhelpful thought? It is handy though, they can interpret exactly the same thought as helpful, or unhelpful, as it suits them. Heads we win, tails you lose.]
Main Body Symptoms
After a few weeks of the activity plan
I feel fed up because I still feel tired with some muscle aches and dizziness
Unhelpful thought
I hardly feel any better and I'm really working a my activity and rest plan
Alternative Thoughts
I know research has shown that with inactivity my body has got physically unfit very quickly...it's logical that it will take time to build up my body again
Main Body Symptoms
After Exercise
I feel like I am relapsing
Unhelpful thoughts
Last time I tried to exercise I became really bad.
Activity or exercise just makes it worse.
Alternative thoughts
Resting hasn't made me better in the past and I don't know if I'll get better or worse doing a gradually controlled activity plan unless I try it. However, others have recovered in this way.
Pain is normal if i exercise when I'm so unfit. But if I keep on exercising at the right level, I will build up stamina and fitness as an athelete does and pain will slowly disappear
[Orla - we wish. There is no evidence for this view. Notice that they are comparing ME/CFS pain with the normal exercise pain an unfit person would get.
I just love the manipulation on the rest and recovery thing. Just because one may not recover with rest, doesn't mean it hasn't a place in management (even they advocate rest periods elsewhere in the document, mind you it is rest but not as we know it!). Most people mark rest as one of the things they found most helpful. A survey (n=2338) conducted for the UK Chief Medical Officer's working group on ME/CFS found that Rest was considered the most helpful strategy, with 91% finding it helpful.
As for saying others had recovered through GET, this is the clinic where they say people are recoverd when they are not.
And one doesn't necessarily have to do GET before deciding whether it is likely to he helpful, useless or harmful. If one is already doing what one can, and not phobically avoiding activity, has flu-like symptoms etc, then there is no evidence that GET is useful (well there is no good evidence it works for ME/CFS at all actually, if one looks at the objective data). And a person can also look at the research, as well as their own experience, to make an informed decision]