pattismith
Senior Member
- Messages
- 3,946
very valuable article, with many interest for us and a great experience behind.
Neuropathic corneal pain is evoked from both peripheral and central perspective, and both from local and systemic origin.
Neuropathic corneal pain is evoked from both peripheral and central perspective, and both from local and systemic origin.
NEUROPATHIC CORNEAL PAIN (NCP): APPROACHES FOR MANAGEMENT
Gabriela Dieckmann, MD,1,2 Sunali Goyal, MD,3 and Pedram Hamrah, MD, FACS1,2
Abstract
Neuropathic pain is caused by a primary lesion or dysfunction of the nervous system and can occur in the cornea.
However, neuropathic corneal pain (NCP) is currently an ill-defined disease.
Patients with NCP are extremely challenging to manage and evidence-based clinical recommendations for the management of patients with NCP are scarce.
The objectives of this review are to provide guidelines for diagnosis and treatment of patients with NCP and to summarize current evidence-based literature in this area.
We performed a systematic literature search of all relevant publications between 1966 and 2017.
Treatment recommendations are, in part, based on methodologically sound randomized controlled trials (RCTs), demonstrating superiority to placebo or relevant control treatments, and on the consistency of evidence, degree of efficacy, and safety.
In addition, the recommendations include our own extensive experience in the management of these patients over the past decade.
A comprehensive algorithm, based on clinical evaluation and complementary tests, is presented for diagnosis and subcategorization of patients with NCP.
Recommended first-line topical treatments include neuro-regenerative and anti-inflammatory agents, whilst first-line systemic pharmacotherapy includes tricyclic antidepressants and the anticonvulsant.
Second line oral treatments recommended include the opioid-antagonist and opiate analgesics.
Complementary and alternative treatments, such as cardio-exercise, acupuncture, omega-3 fatty acid, and gluten-free diet, may have additional benefits, as do potential non-invasive and invasive procedures in recalcitrant cases.
Medication selection should be tailored on an individual basis, considering side effects, comorbidities, and levels of peripheral and centralized pain.
Nevertheless, there is an urgent need for long-term studies and RCTs assessing the efficacy of treatments for NCP.
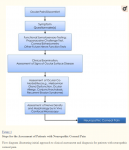
The Proparacaine Challenge Test
Establishing the origin of pain, whether central or peripheral is important for selecting appropriate treatment measures. Topical 0.5% proparacaine hydrochloride (Alcaine, Alcon, Fort Worth, TX) allows for differentiation of central from peripheral sources of pain.13 While proparacaine abolishes peripheral pain, it has no effect on pain from central sensitization. Patients experiencing complete or partial relief with proparacaine challenge, likely suffer from peripheral or mixed combined NCP. In contrast, patients not responding to proparacaine, suffer at least in part from central NCP (Fig. 2). It has been our clinical experience that many patients only achieve partial relief to topical proparacaine, suggesting that both peripheral and central sensitization are at play, albeit in different proportions depending on etiology and disease duration.

In Vivo Confocal Microscopy to Confirm Corneal Nerve Damage
The cornea is innervated by branches of the nasociliary nerve, a branch of the ophthalmic division of the trigeminal nerve.43 Nerve bundles enter the peripheral cornea (limbus) in a radial fashion, migrate anteriorly, penetrate the Bowman’s layer, and form the subbasal plexus.
Neuro-Regenerative Therapy
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5743225/#R51Peripheral sensitization in NCP is initiated by corneal nerve injury and subsequent inflammation. Recently, therapeutic strategies targeting neuronal regeneration have been shown to alleviate patient symptoms with autologous serum tears (AST).6 The rationale for this approach was based on previous reports from preclinical non-ocular neuropathic pain models on the use of neurotrophic factors, in particular nerve growth factor (NGF).47,48 NGF reduced allodynia and hyperalgesia through reduction of reactive astrocytosis and glial modulation. Recovery of corneal nerve topography has been demonstrated with the use of AST in patients with NCP,49 photoallodynia,6 DED,50 as well as with autologous plasma in patients with neurotrophic keratopathy.51
Autologous Serum Tears (AST)
AST contain neurotrophic factors, including NGF and insulin-like growth factor ....
We recommend the use of 20% AST 8x/daily until significant relief/resolution of symptoms is achieved, followed by a very slow taper in order to prevent rebound. It has been our experience that initial symptom relief is observed within 3–4 months in NCP of peripheral origin and that taper can be successfully attempted within 9–12 months
Anti-Inflammatory Therapy
The pathophysiology of NCP includes injury to peripheral nerves (e.g. due to direct trauma, inflammation, toxicity) resulting in release of pro-inflammatory neuropeptides from both injured nerves and cytokines from surrounding healthy nerves,71,72 leading peripheral sensitization.73,74
Chronic inflammation can decrease neurite outgrowth and increased calcium influx across cell membranes, causing axonal degeneration.75,76 Thus, the critical role of inflammation in the pathophysiology of NCP provides the rationale for the use of anti-inflammatory therapy. Our clinical experience has corroborated this rationale in that concurrent use of low dose topical corticosteroids with AST resulted in significant increase in cornea nerve regeneration as compared to AST alone.
Topical corticosteroids have been used as a mainstay of anti-inflammatory therapy due to their inhibitory mechanism of action on cytokines, prostaglandins and leukotriene synthesis, as well as the inhibition of leukocyte migration.78
Among corticosteroids, loteprednol 0.5% suspension or gel have demonstrated lower rates of increased intraocular pressure and cataract formation due to decreased intraocular penetration.79, 80 Moreover loteprednol 0.5% gel has a much lower concentration of the neurotoxic81–83 preservative benzalkonium chloride (BAK; 0.003%), as compared to other corticosteroids;
Thus, for NCP we recommend use of loteprednol 0.5% suspension or gel with a slow taper of four times daily for two weeks, followed by twice daily for two weeks and once daily over a 6- to 12-week period depending on individual patient response. Anti-inflammatory therapy is then attempted with steroid-sparing therapies, such as topical calcineurin inhibitors cyclosporine A 0.05% two to four times daily,86 and tacrolimus 0.03% three times daily,87 the interleukin-1 receptor antagonist Anakinra (Kineret) 2.5% three times daily,88 as well as topical testosterone 0.03% three times daily.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5743225/#R51