It would be interesting to know why Goldstein was not interested in inosine, while many other CFS/ME doctors seem to use it a lot.
Inosine has different effects:
-binding to adenosine receptors outside the cell
-activities inside the cell
-catabolism inside the cell, leading to urate production via xanthine oxidase
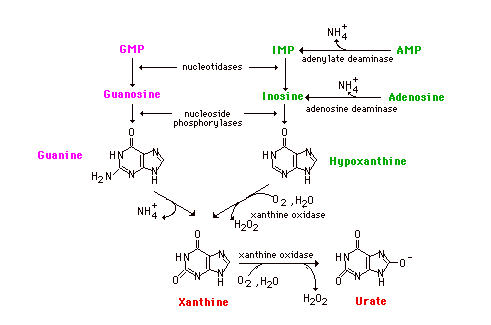
Modulation of Inosine activity could be done
-either by adding a xanthine oxidase inhibitor (Allopurinol, or a more natural one for example Quercitin) in order to reduce the Urate production
-either by taking Dipirydamole in order to increase the effect on adenosine receptors and reduce the urate production.
Inosine is doing a great job for me (on pain and mood disorders) by binding to adenosine receptors, but I feel concerned that it may increase too much my blood urate, so I think about exploring these two possibilities.
Thank you for bringing it to me!
Good! I'm glad to hear its helping. You have to remember that Goldstein wrote his books a very long time ago. Most supplements were still pretty unknown back then.
I don't know if you have Goldstein's book or his algorithm. My copy is falling apart into separate pages now from being opened so many times over the years, I need to figure out where I can get it bound (this book holds a sentimental value for me).
His algorithm basically went in this order:
ALPHA 2 RECEPTORS (profiled with naphazoline eye drops, may be able to buy in the pharmacy)
Starting with alpha-2 receptors agonist or antagonist based on response to naphazoline eye drops.
BETTER: clonidine, gunfacine (Intuniv), midodrine, reboxetine
WORSE: Buspirone, mirtazapine (my note: I would add mianserin too; low doses of mianserine and mirtazapine are more sedating than high doses due to H1 effect)
TRH (this is hard to get; there is Abaris which is sublingual TRH but I don't know if it works the same way.
Response to TRH drops which IMO could be "estimated in reverse" by T3 causing TRH suppression. Some people use TSH suppression protocols for T3 but I actually feel really bad if my TSH is suppressed. If people were feeling worse with TRH spray, for Goldstein it was a predictor they would do well with adenosine.
You were able to tolerate T3 (TRH suppression) much better than I could so it makes sense that you respond to adenosine. I seem to need a decent level of TRH to function well and I think adenosine (based on my Cordyceps response) generally makes me worse.
BETTER WITH TRH: DHEA, Aricept, cycloserine, modafinil, Talwin, dopamine
WORSE WITH TRH: gotu kola, dipyridamole, baclofen, taurine, gabapentin and benzos.
DOPAMINE (profiled with dopamine drops but might be able to interpolate from other agensts, like Ritalin):
BETTER: Forskolin, naltrexone, THC, testosterone, oxytocin, reboxetine, selegiline, ropinirole, oxytocin, hydergine, amantadine
WORSE: mestinon, nimotop, piracetam, risperidal, Ativan, verapamil
ADENOSINE DROPS
Better: adenosine, ascorbate, Buspar, EFAs, guafenesin, heparin, L-lysine, lidocaine, progesterone, Topamax, Nimotop, gabapentin, mecamylamine (note that he lists L-lysine and lysine separately)
Worse: cycloseine, DHEA, pregnenolone, taurine, testosterone, lamotrigine, piracetam, tramadol
At this point he tests ketamine, lidocaine, amantadine and gabapentin) and algorithm becomes somewhat useless as it basically jumps between the same two columns full of meds until he comes back with specific NDMA drugs:
NDMA RECEPTOR (judged by the response to guafenesin topical gel)
BETTER: diltiazem, Nimotop, Zofran
WORSE: cycloserine, high dose glycine/serine.
My only residual issue right now is sort of general lassitude (not the same as fatigue) and lack of motivation - which could be because I didn't address alpha2 adrenergic receptors and I don't have enough NE. Or it could be because my TRH is still too suppressed which again would result in low catecholamines. Or maybe I need to get my hands on some cycloserine to bump up my NDMA function (I couldn't find it but ordered some sarcosine yesterday which is used for the same purposes).
On the bright side, all my pain, dysautonomia and mood problems are pretty much resolved and I can tolerate most drugs and supplements without any problem.

