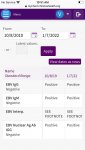
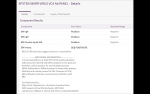
I'm really angry that my oncologist didn't follow up on positive EBV IgM in 2019. She'd ordered dozens of tests at that time, and I think was more focused on the cancer-related ones (including PET scan) due to recurrent fevers and lymphadenopathy. I wasn't even aware of the positive IgM result until mid-2021, when my new immunologist noticed it while reviewing my medical record. His advice at the time was to get another EBV IgG/IgM antibody test if I experienced another episode of fever and lymphadenopathy, which was just this past week
I have been in the cancer survivor system in 2 major US cities, both known for their high quality cancer care. I was sleeping 16 hours a day I couldn't see straight or think straight in 2016, and went to over a dozen MDs and the cancer community saying I thought there was something wrong with my immune system and could someone please help me find answers. I got gaslighted, had head shaking, and the best offer I got was to go to a pain clinic when I wasn't in pain.
Meanwhile, my naturopathic doctor was busily running standard LabCorp tests and found the HHV6 and cytomegalovirus and enough wrong with my immune system that I sought out a top specialist in another state, who found the EBV that everyone else had missed by doing a PCR test as well as 6 other chronic infections and significant immunodeficiency. Treating each of these has greatly helped.
Feeling stable, I moved across the country, to be turned down by 6 primary care practices sight unseen, because "you're too complex." Both the old and the new cancer survivorship clinics told me that cancer survivors have real problems in getting good care because the primary care doctors just don't understand the complexity of what we're dealing with and the cancer people think they're done with us because they've saved our lives by curing the cancer. Meanwhile, the rest of the medical system is so super specialized that the kidney doctors only look at kidneys, the neurologists only look at brains, the cardiologists only look at hearts, etc.
I've also found immunologists which tend to be a strange lot. Most of them that we have access to are allergy specialists, so dealing with a patient with a chronic virus and even immunodeficiency isn't in their normal realm, which is allergy shots and treating asthma. There are cancer immunologists, but they don't want to deal with a likes of us, they tinker with the immune system to get it to kill cancers. Then, there are the AIDS immunologists, which, ironically, can be the best for us, because they have seen immune systems go haywire with all kinds of weird opportunistic infections and immunodeficiency, so they are better equipped to help us, although usually we can't see them.
Then there are infectious disease doctors. I have yet to have one help me. They seem to be more interested in rare tropical diseases that we get on vacation or bacterial infections, I guess, but they seem to be lousy at dealing with EBV, HHV6, and CMV Not to mention prescribing an antiviral. I had one helpfully test me for tuberculosis and syphilis, neither of which I had any reason to suspect I had, But miss the EBV.
Rheumatologists are also a strange lot. I don't know what they do. I wasted a lot of time waiting for appointments with one only to have her fire me when she couldn't figure out how to help me. She also missed the EBV, refused to look at my HHV6 and CMV, and couldn't find the multiple types of autoimmunity that I had. A lot of them put people on immunosuppressive drugs that lead to leukemia and lymphomas.
So, I think the best doctor is one who cares about your symptoms, is curious, and willing to entertain more oddball diagnoses And is willing to look at any scientific paper you bring thoughtfully and provide solutions.
Given what you have shared, it seems that you have had an EBV infection that your body has not cleared. You need treatment. Once my EBV was found, my doctor wanted to put me on 3g valacyclovir (Valtrex) daily, but my insurance denied that dose and would only let me have 2g and because I also had active HHV6 and CMV, valganciclovir was the better drug, and he put me on 4 450mg pills daily for 12 months and 2 450mg daily for another 8 months until I had 4 successive negative PCR tests.
He also supported my immune system with low dose naltrexone (4.5mg) and intravenous immunoglobulins, which I still get every three weeks.
I've been having autoimmune illness symptoms for years, without definitive diagnosis. I was last tested for ANA in 2019 and was negative. As for Rheumatoid Arthritis I am positive for CCP but negative for RA factor (also last tested in 2019), and don't have enough other clinical symptoms to have gotten an RA diagnosis officially, but my doctors have mentioned it as "possible." I cannot count the number of times I have been tested for leukemia because of symptoms, and high risk due to radiation/chemo, but those tests have always been negative.
EBV is notorious for triggering autoimmune disease. This, in addition to the cancer causing potential for EBV, is why treating it earlier rather than later is wise.
I've also attached a list of antibody tests collected from patients on this forum. EBV is not specific in what it triggers, so you might look through the list and see if you have any sorts of symptoms associated with the antibodies. If you're lucky, you get well recognized antibodies that doctors feel comfortable treating. If you're really unlucky you can end up with autoimmune encephalitis which has killed patients. Somewhere in between are those of us with autoimmune POTS which no US lab tests for, but that a good German one does, and then US doctors refuse to recognize it because it wasn't run in the US...
If I were in your shoes, I would take your previous test results, the orange chart I posted above, and talk to your immunologist, and ask to be put on valacyclovir while being tested for other herpes family viruses, with both antibody and PCR tests. I would also ask for a thorough look at your immune system, including immunoglobulins, NK cell function, CD4/CD8. And, if this doctor refuses, I would be persistent and finding a doctor who will help you, whether it's in internal medicine doctor or one of the other ones that I listed.
After that is accomplished, I would look at antibody testing and see what's going on. If you have multiple nasty antibodies that are causing a significant problems, there are some specialists who would prescribe IVIG for a while, treat any infections they can possibly find, and then prescribe a course of rituximab, which is about a year process, which can wipe out the B cells causing the bad antibodies, before letting them eventually grow back, hopefully not producing antibodies. This strategy helped a few of us. But there's a lot of other work that must happen first.
You deserve help and to the bottom of this.