Cipher
Administrator
- Messages
- 862
A Tough Nut to Crack: Chronic Fatigue Syndrome and Abdominal Pain Attributed to Nutcracker Syndrome
DOI: 10.15761/IMC.1000101
Abstract
Nutcracker phenomenon refers to entrapment of the left renal vein between the superior mesenteric artery and aorta. This can result in elevated left renal vein pressure and reduced renal perfusion. Nutcracker syndrome, which refers to symptoms associated with the above phenomenon, usually presents with acute onset hematuria and abdominal pain, but more rarely, may present as chronic fatigue syndrome. Here, we present a case of a 24-year-old male with a seven-year history of chronic fatigue syndrome, which was subsequently found to have imaging characteristics consistent with nutcracker phenomenon. His fatigue markedly improved after insertion of a left renal vein stent.
Introduction
Nutcracker phenomenon is a rare condition. It refers to compression of the left renal vein between the abdominal aorta and superior mesenteric artery. The entrapment of the left renal vein causes distention of the distal portion of the vein, elevated venous pressure and reduced renal perfusion with formation of prominent collateral vessels. The term nutcracker syndrome (NS) refers to symptoms that arise from the nutcracker phenomenon. Sometimes these terms are used interchangeably, but it has been emphasized [1] that the term nutcracker syndrome should be reserved for patients with the characteristic clinical symptoms in association with demonstrable radiographic findings. Furthermore, not all patients with the radiographic findings of nutcracker phenomenon will have clinical symptoms [2]. There is a wide spectrum of common clinical presentations for NS. However, symptoms usually include hematuria and abdominal pain [3]. One very rare presentation of NS is chronic fatigue syndrome which has been reported in pediatric literature [4], but not yet, to our knowledge, in adult literature. Chronic fatigue syndrome (CFS) can be a debilitating condition characterized by persistent fatigue and an impairment in ability to engage in daily activities for more than six months (three months in children and adolescents), with post-exertional malaise, unrefreshing sleep, and must be associated with either cognitive impairment or orthostatic intolerance. It is a clinical diagnosis of exclusion [5,6]. Here, we report the case of a patient with CFS diagnosed seven years prior who presented to our institution with worsening abdominal pain. Computed tomography (CT) revealed nutcracker phenomenon. He subsequently underwent left renal vein stent insertion with improvement of both fatigue and abdominal pain. To our knowledge, this is the first reported case of chronic fatigue syndrome attributable to NS in an adult.
Case report
A 24-year-old male presented to our institution with worsening abdominal pain in the setting of a seven-year history of chronic fatigue syndrome, chronic pelvic pain syndrome, and vague abdominal pain. He was healthy until age 17, when he noted abrupt onset fatigue and orthostasis. His symptoms were severe enough to prevent him from exercise and keeping a job. He was evaluated by multiple physicians, but no satisfactory diagnosis was made. A tilt table test showed a possible tachycardic response, and a trial of fludrocortisone was initiated, with only mild improvement in symptoms. Dextroamphetamine/amphetamine was also tried for fatigue, also with limited response. At the time of hospitalization, his pain was nonspecific and primarily limited to the left side of his abdomen. Pain was exacerbated while in the standing position, and with walking, He described it as “stabbing and gnawing” pain that occasionally worsened after eating and at night time. Pain was not associated with nausea, vomiting, dysuria, or a change in bowel habits. He also complained of intermittent, progressively worsening fatigue, described “slowed thinking” and inability to exercise without feeling lightheaded. Physical examination was normal, and there was no stigma of chronic disease. Symptoms persisted despite conservative therapy, and he reported new onset dysuria and dark urine. Subsequent abdominal and pelvis computed tomography (CT) revealed compression of the left renal vein between the aorta and superior mesenteric artery (Figure 1). Vascular surgery was consulted; the diagnosis of nutcracker syndrome was made and surgical intervention was recommended. He underwent surgery and left renal vein stent placement (Figure 2). His symptoms resolved soon after intervention.
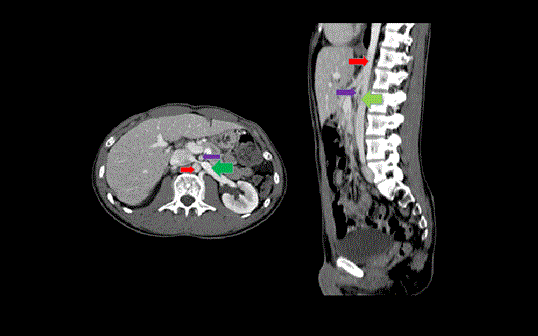
Figure 1: Computed topographic venogram showing nutcracker phenomenon. Left renal vein with distended hilar portion (green arrow) is compressed between the aorta (red arrow) and the superior mesenteric artery (blue arrow).
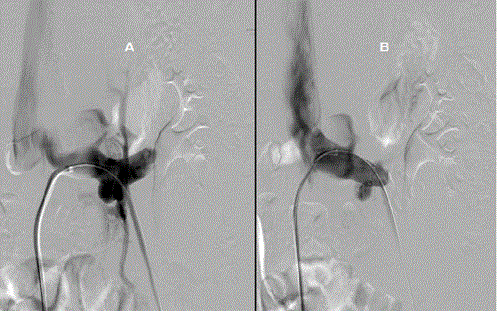
Figure 2: A. Pre-stent contrast injection directly into the left renal vein demonstrated delayed/decreased flow into the IVC due to stenosis at the origin of the renal vein. Since there is decreased drainage into the IVC, the renal vein alternatively partially empties into a prominent lumbar collateral vein. B. Post-stent contrast injection demonstrated resolution of stenosis with improved drainage of the left renal vein into the IVC and lack of flow in the previously seen collateral vessel.
Discussion
Nutcracker syndrome (NS) is the constellation of symptoms associated with left renal vein entrapment because of nutcracker phenomenon [7,8]. Its natural history is not well understood and there is a wide spectrum of clinical presentations. The exact prevalence of NS is unknown due to the variability of symptoms and absence of diagnostic criteria, but it is thought to be under-diagnosed [2]. Age at presentation can range from childhood to the seventh decade, but most symptomatic patients typically present in the second or third decade [7]. The frequency and severity of symptoms varies, but usually includes microscopic hematuria [9] and abdominal pain [10]. Other possible manifestations include gonadal vein syndrome [11], varicoceles [12], orthostatic proteinuria [13], and orthostatic intolerance [14]. Chronic fatigue syndrome is a very rare manifestation that has, to our knowledge, only been reported in pediatric literature thus far [4]. Hematuria from NS is attributed to elevated venous pressures leading to rupture of the thin-walled veins into the collecting system or between dilated venous sinuses and adjacent renal calyces [16]. It ranges from microscopic to gross hematuria, rarely with resultant anemia that requires blood transfusions [17]. In one study by Shin et al [18], the etiology of isolated hematuria was not identified by routine methods in 69% of pediatric cases. Further investigation with renal Doppler ultrasonography identified 40% of those to have nutcracker phenomenon. Pain, the second most common symptom in NS, is often described as colicky with radiation to the posteromedial thigh and buttock [2]. Symptoms are often aggravated by certain postures, and by physical activity such as standing, walking, and riding a bicycle [14,19]. Pain is thought to be more prominent in the upright and supine positions because of visceral proptosis and a change of the aorto-mesenteric angle [20]. Left flank pain also may be attributed to left ureteral colic due to the passing of blood clots through the left ureter [2]. Since the left gonadal veins drain via the left renal vein, this may also present as testicular pain in men, and left lower quadrant abdominal pain in women. Chronic fatigue syndrome (CFS) is characterized by profound fatigue and a combination of several other symptoms that can result in significant morbidity [21]. Multiple biologic, genetic, infectious and psychological mechanisms have been proposed, but the etiologyof CFS is still not well-understood, and it may be multifactorial [6,21]. The association between fatigue and NS is not well understood, but is thought to involve an elevated left renal vein–inferior vena cava pressure gradient [2]. The degree of fatigue has been positively correlated with high peak velocity ratios in some patients [7]. The gold standard for the diagnosis of nutcracker phenomenon is renal venography combined with measurement of renocaval pressure gradient, but currently there is no consensus on diagnostic criteria [16]. Abdominal CT and ultrasonography have also been found to be useful [16]. Variants of normal anatomy and effect of posture must be considered before making the diagnosis. For instance, significant differences in left renal vein diameter at the aorto-mesenteric portion have been demonstrated between the supine and upright positions [19]. It can be difficult to correlate imaging results and symptoms, thus treatment is only recommended for patients with severe or persistent symptoms [12]. For patients younger than 18 years, observation for at least two years is recommended because up to 75% of patients may have complete spontaneous resolution of hematuria [2]. Medical management with angiotensin inhibitors [19,22] or aspirin [23] may also be appropriate for select patients. Stenting and open surgical interventions are both appropriate treatment options that can provide significant long-term, symptomatic relief for patients with NS. Stenting is a more relatively recent utilized technique with good outcomes [24], but long-term follow-up data are currently lacking. Stenting is generally well tolerated, and some patients have been successfully managed with aspirin or clopidogrel without long-term anticoagulation [25]. In conclusion, NS is a rare diagnosis that usually presents with acute onset hematuria and abdominal pain. It should be considered in the differential diagnosis of chronic fatigue syndrome associated with abdominal pain.
References
DOI: 10.15761/IMC.1000101
Abstract
Nutcracker phenomenon refers to entrapment of the left renal vein between the superior mesenteric artery and aorta. This can result in elevated left renal vein pressure and reduced renal perfusion. Nutcracker syndrome, which refers to symptoms associated with the above phenomenon, usually presents with acute onset hematuria and abdominal pain, but more rarely, may present as chronic fatigue syndrome. Here, we present a case of a 24-year-old male with a seven-year history of chronic fatigue syndrome, which was subsequently found to have imaging characteristics consistent with nutcracker phenomenon. His fatigue markedly improved after insertion of a left renal vein stent.
Introduction
Nutcracker phenomenon is a rare condition. It refers to compression of the left renal vein between the abdominal aorta and superior mesenteric artery. The entrapment of the left renal vein causes distention of the distal portion of the vein, elevated venous pressure and reduced renal perfusion with formation of prominent collateral vessels. The term nutcracker syndrome (NS) refers to symptoms that arise from the nutcracker phenomenon. Sometimes these terms are used interchangeably, but it has been emphasized [1] that the term nutcracker syndrome should be reserved for patients with the characteristic clinical symptoms in association with demonstrable radiographic findings. Furthermore, not all patients with the radiographic findings of nutcracker phenomenon will have clinical symptoms [2]. There is a wide spectrum of common clinical presentations for NS. However, symptoms usually include hematuria and abdominal pain [3]. One very rare presentation of NS is chronic fatigue syndrome which has been reported in pediatric literature [4], but not yet, to our knowledge, in adult literature. Chronic fatigue syndrome (CFS) can be a debilitating condition characterized by persistent fatigue and an impairment in ability to engage in daily activities for more than six months (three months in children and adolescents), with post-exertional malaise, unrefreshing sleep, and must be associated with either cognitive impairment or orthostatic intolerance. It is a clinical diagnosis of exclusion [5,6]. Here, we report the case of a patient with CFS diagnosed seven years prior who presented to our institution with worsening abdominal pain. Computed tomography (CT) revealed nutcracker phenomenon. He subsequently underwent left renal vein stent insertion with improvement of both fatigue and abdominal pain. To our knowledge, this is the first reported case of chronic fatigue syndrome attributable to NS in an adult.
Case report
A 24-year-old male presented to our institution with worsening abdominal pain in the setting of a seven-year history of chronic fatigue syndrome, chronic pelvic pain syndrome, and vague abdominal pain. He was healthy until age 17, when he noted abrupt onset fatigue and orthostasis. His symptoms were severe enough to prevent him from exercise and keeping a job. He was evaluated by multiple physicians, but no satisfactory diagnosis was made. A tilt table test showed a possible tachycardic response, and a trial of fludrocortisone was initiated, with only mild improvement in symptoms. Dextroamphetamine/amphetamine was also tried for fatigue, also with limited response. At the time of hospitalization, his pain was nonspecific and primarily limited to the left side of his abdomen. Pain was exacerbated while in the standing position, and with walking, He described it as “stabbing and gnawing” pain that occasionally worsened after eating and at night time. Pain was not associated with nausea, vomiting, dysuria, or a change in bowel habits. He also complained of intermittent, progressively worsening fatigue, described “slowed thinking” and inability to exercise without feeling lightheaded. Physical examination was normal, and there was no stigma of chronic disease. Symptoms persisted despite conservative therapy, and he reported new onset dysuria and dark urine. Subsequent abdominal and pelvis computed tomography (CT) revealed compression of the left renal vein between the aorta and superior mesenteric artery (Figure 1). Vascular surgery was consulted; the diagnosis of nutcracker syndrome was made and surgical intervention was recommended. He underwent surgery and left renal vein stent placement (Figure 2). His symptoms resolved soon after intervention.

Figure 1: Computed topographic venogram showing nutcracker phenomenon. Left renal vein with distended hilar portion (green arrow) is compressed between the aorta (red arrow) and the superior mesenteric artery (blue arrow).

Figure 2: A. Pre-stent contrast injection directly into the left renal vein demonstrated delayed/decreased flow into the IVC due to stenosis at the origin of the renal vein. Since there is decreased drainage into the IVC, the renal vein alternatively partially empties into a prominent lumbar collateral vein. B. Post-stent contrast injection demonstrated resolution of stenosis with improved drainage of the left renal vein into the IVC and lack of flow in the previously seen collateral vessel.
Discussion
Nutcracker syndrome (NS) is the constellation of symptoms associated with left renal vein entrapment because of nutcracker phenomenon [7,8]. Its natural history is not well understood and there is a wide spectrum of clinical presentations. The exact prevalence of NS is unknown due to the variability of symptoms and absence of diagnostic criteria, but it is thought to be under-diagnosed [2]. Age at presentation can range from childhood to the seventh decade, but most symptomatic patients typically present in the second or third decade [7]. The frequency and severity of symptoms varies, but usually includes microscopic hematuria [9] and abdominal pain [10]. Other possible manifestations include gonadal vein syndrome [11], varicoceles [12], orthostatic proteinuria [13], and orthostatic intolerance [14]. Chronic fatigue syndrome is a very rare manifestation that has, to our knowledge, only been reported in pediatric literature thus far [4]. Hematuria from NS is attributed to elevated venous pressures leading to rupture of the thin-walled veins into the collecting system or between dilated venous sinuses and adjacent renal calyces [16]. It ranges from microscopic to gross hematuria, rarely with resultant anemia that requires blood transfusions [17]. In one study by Shin et al [18], the etiology of isolated hematuria was not identified by routine methods in 69% of pediatric cases. Further investigation with renal Doppler ultrasonography identified 40% of those to have nutcracker phenomenon. Pain, the second most common symptom in NS, is often described as colicky with radiation to the posteromedial thigh and buttock [2]. Symptoms are often aggravated by certain postures, and by physical activity such as standing, walking, and riding a bicycle [14,19]. Pain is thought to be more prominent in the upright and supine positions because of visceral proptosis and a change of the aorto-mesenteric angle [20]. Left flank pain also may be attributed to left ureteral colic due to the passing of blood clots through the left ureter [2]. Since the left gonadal veins drain via the left renal vein, this may also present as testicular pain in men, and left lower quadrant abdominal pain in women. Chronic fatigue syndrome (CFS) is characterized by profound fatigue and a combination of several other symptoms that can result in significant morbidity [21]. Multiple biologic, genetic, infectious and psychological mechanisms have been proposed, but the etiologyof CFS is still not well-understood, and it may be multifactorial [6,21]. The association between fatigue and NS is not well understood, but is thought to involve an elevated left renal vein–inferior vena cava pressure gradient [2]. The degree of fatigue has been positively correlated with high peak velocity ratios in some patients [7]. The gold standard for the diagnosis of nutcracker phenomenon is renal venography combined with measurement of renocaval pressure gradient, but currently there is no consensus on diagnostic criteria [16]. Abdominal CT and ultrasonography have also been found to be useful [16]. Variants of normal anatomy and effect of posture must be considered before making the diagnosis. For instance, significant differences in left renal vein diameter at the aorto-mesenteric portion have been demonstrated between the supine and upright positions [19]. It can be difficult to correlate imaging results and symptoms, thus treatment is only recommended for patients with severe or persistent symptoms [12]. For patients younger than 18 years, observation for at least two years is recommended because up to 75% of patients may have complete spontaneous resolution of hematuria [2]. Medical management with angiotensin inhibitors [19,22] or aspirin [23] may also be appropriate for select patients. Stenting and open surgical interventions are both appropriate treatment options that can provide significant long-term, symptomatic relief for patients with NS. Stenting is a more relatively recent utilized technique with good outcomes [24], but long-term follow-up data are currently lacking. Stenting is generally well tolerated, and some patients have been successfully managed with aspirin or clopidogrel without long-term anticoagulation [25]. In conclusion, NS is a rare diagnosis that usually presents with acute onset hematuria and abdominal pain. It should be considered in the differential diagnosis of chronic fatigue syndrome associated with abdominal pain.
References
- Shin JI, Lee JS (2005) Nutcracker phenomenon or nutcracker syndrome? Nephrol Dial Transplant 20: 2015. [Crossref]
- Kurklinsky AK, Rooke TW (2010) Nutcracker phenomenon and nutcracker syndrome. Mayo Clin Proc 85: 552-529.
- Shin JI, Lee JS, Kim MJ (2006) The prevalence, physical characteristics and diagnosis of nutcracker syndrome. Eur J Vasc Endovasc Surg 32: 335-336.
- Takahashi Y, Ohta S, Sano A, Kuroda Y, Kaji Y, et al. (2000) Does severe nutcracker phenomenon cause pediatric chronic fatigue. Clin Nephrol 53: 174-181.
- Sanders P, Korf J (2008) Neuroaetiology of chronic fatigue syndrome: an overview. World J Biol Psychiatry 9: 165-171.
- Afari N, Buchwald D (2003) Chronic fatigue syndrome: a review. Am J Psychiatry 160: 221-36.
- Rudloff U, Holmes RJ, Prem JT, Faust GR, Moldwin R, et al. (2006) Mesoaortic compression of the left renal vein (nutcracker syndrome): case reports and review of the literature. Ann Vasc Surg 20: 120-129.
- Cope C, Isard HJ (1969) Left renal vein entrapment. A new diagnostic finding in retroperitoneal disease. Radiology 92: 867-872.
- Oteki T, Nagase S, Hirayama A, Sugimoto H, Hirayama K, et al. (2004) Nutcracker syndrome associated with severe anemia and mild proteinuria. Clin Nephrol 62: 62-65.
- Rogers A, Beech A, Braithwaite B et al. (2007) Transperitoneal laparoscopic left gonadal vein ligation can be the right treatment option for pelvic congestion symptoms secondary to nutcracker syndrome. Vascular 15: 238-240.
- Coolsaet BL (1978) Ureteric pathology in relation to right and left gonadal veins. Urology 12: 40-49.
- Park SJ, Lim JW, Ko YT, Lee DH, Yoon Y, et al. (2004) Diagnosis of pelvic congestion syndrome using transabdominal and transvaginal sonography. AJR Am J Roentgenol 182: 683-688.
- Shintaku N, Takahashi Y, Akaishi K, Sano A, Kuroda Y (1990) Entrapment of left renal vein in children with orthostatic proteinuria. Pediatr Nephrol 4: 324-327.
- Takahashi Y, Sano A, Matsuo M (2005) An ultrasonographic classification for diverse clinical symptoms of pediatric nutcracker phenomenon. Clin Nephrol 64: 47-54.
- Shin JI, Park JM, Lee SM, Shin YH, Kim JH, et al. (2005) Factors affecting spontaneous resolution of hematuria in childhood nutcracker syndrome. Pediatr Nephrol 20: 609-613.
- Takebayashi S, Ueki T, Ikeda N, Fujikawa A (1999) Diagnosis of the nutcracker syndrome with color Doppler sonography: correlation with flow patterns on retrograde left renal venography. AJR Am J Roentgenol 172: 39-43.
- Segawa N, Azuma H, Iwamoto Y, Sakamoto T, Suzuki T, et al. (1999) Expandable metallic stent placement for nutcracker phenomenon. Urology 53: 631-663.
- Shin JI, Park JM, Lee JS, Kim MJ (2007) Effect of renal Doppler ultrasound on the detection of nutcracker syndrome in children with hematuria. Eur J Pediatr 166: 399-404.
- Fitoz S, Ekim M, Ozcakar ZB, Elhan AH, Yalcinkaya F, et al. (2007) Nutcracker syndrome in children: the role of upright position examination and superior mesenteric artery angle measurement in the diagnosis. J Ultrasound Med 26: 573-80.
- Sayfan J, Halevy A, Oland J, Nathan H (1984) Varicocele and left renal vein compression. Fertil Steril 41: 411-417.
- Griffith JP, Zarrouf FA (2008) A systematic review of chronic fatigue syndrome: don't assume it's depression. Prim Care Companion J Clin Psychiatry 10: 120-128.
- Urban BA, Ratner LE, Fishman EK (2001) Three-dimensional volume-rendered CT angiography of the renal arteries and veins: normal anatomy, variants, and clinical applications. Radiographics 21: 373-86.
- Scholbach T (2007) From the nutcracker-phenomenon of the left renal vein to the midline congestion syndrome as a cause of migraine, headache, back and abdominal pain and functional disorders of pelvic organs. Med Hypotheses 68: 1318-1327.
- Policha A, Lamparello P, Sadek M, Berland T, Maldonado T (2016) Endovascular Treatment of Nutcracker Syndrome. Ann Vasc Surg.
- Hartung O, Grisoli D, Boufi M, Marani I, Hakam Z, et al. (2005) Endovascular stenting in the treatment of pelvic vein congestion caused by nutcracker syndrome: lessons learned from the first five cases. J Vasc Surg 42: 275-280.
