-

Welcome to Phoenix Rising!
Created in 2008, Phoenix Rising is the largest and oldest forum dedicated to furthering the understanding of, and finding treatments for, complex chronic illnesses such as chronic fatigue syndrome (ME/CFS), fibromyalgia, long COVID, postural orthostatic tachycardia syndrome (POTS), mast cell activation syndrome (MCAS), and allied diseases.
To become a member, simply click the Register button at the top right.
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Guys Let's Focus on the latest science here
- Thread starter eljefe19
- Start date
Jonathan Edwards
"Gibberish"
- Messages
- 5,256
Also, if you do not think the term should be used in this context, would you therefore say that it is not possible/useful to broadly characterise the differences between the immune systems of different individuals, sexes, or species?
It's all imunobabble, msf. There is no such thing as a net balance of cytokines. Most cytokines contribute both positively and negatively to inflammatory events in various ways. A carpenter does not talk of 'tool balance' in his toolbag. He uses each tool for a different purpose.
Ok, breaking it down, so no one misunderstands anyone. Do patients suffering from diseases thought of as causing inflammation have an immunosignature? If so, surely that immunosignature would partly be made up of differing levels of cytokines. If so, it should be the case that some people with those diseases would have levels of those cytokines that are more typical for that group, and others would have levels of those cytokines that are more typical of controls. If we then say that those with the typical levels have an more inflammatory response, and those with the levels more typical of controls have a less inflammatory (or anti-inflammatory) response, do we need to quibble about the terminology? I know Prof. Edwards will now say that no generalisations can be made about the type of disease, but has that actually been established? It would seem to me that it hasn´t, and that is why researchers test for things like TNF-a and IFNy when they suspect that an ´inflammatory event´ might be present in a disease that they do not presently understand. There are other cytokines that might be less strongly associated with diseases in which there are inflammatory events, but that does not invalidate the whole concept, but rather requires that the model be tweaked to weigh each cytokine separately. If it then turns out that no useful predictions can be made about what type of disease is present, then it would not be a useful concept, but I really doubt that this has been properly evaluated, and it seems to be much more likely that researchers use these concepts because (even though they might not be well evidenced) the researchers see them as a useful tool (or mental framework) for thinking about what kind of problem they are actually looking at. Whether it is a useful tool or not is also unlikely to have been evaluated.
Jonathan Edwards
"Gibberish"
- Messages
- 5,256
Dear msg,
I cannot work out what you are wanting to hang on to . TH1/TH2 has nothing to do with inflammatory/anti-inflammatory. If anything TH1 is to do with promoting direct T cell mediated response and TH2 has to do with indirect B (via T) cell mediated responses. But the concept collapsed when it became clear that cytokines in both groups contribute to both in different ways. There are researchers who still use these concepts because they have no clue but so what? Jo Cambridge was telling me about the IimE colloquium today. She met an old friend who is a distinguished immunologist who had come along because the British Society for Immunology has got wind of ME/CFS being interesting - which is good news. She was impressed by the hard work and enthusiasm but she and Jo had a mutual moan about how so many colleagues are stuck with ideas from the 1990s - and not very good ones at that.
TNF alpha and IL-1 and IL-6 are often good signs of cytokine mediated inflammation, no one will dispute that, but TH1/TH2 balance is drivel.
I cannot work out what you are wanting to hang on to . TH1/TH2 has nothing to do with inflammatory/anti-inflammatory. If anything TH1 is to do with promoting direct T cell mediated response and TH2 has to do with indirect B (via T) cell mediated responses. But the concept collapsed when it became clear that cytokines in both groups contribute to both in different ways. There are researchers who still use these concepts because they have no clue but so what? Jo Cambridge was telling me about the IimE colloquium today. She met an old friend who is a distinguished immunologist who had come along because the British Society for Immunology has got wind of ME/CFS being interesting - which is good news. She was impressed by the hard work and enthusiasm but she and Jo had a mutual moan about how so many colleagues are stuck with ideas from the 1990s - and not very good ones at that.
TNF alpha and IL-1 and IL-6 are often good signs of cytokine mediated inflammation, no one will dispute that, but TH1/TH2 balance is drivel.
Well, I was just defending idea of a proinflammatory/antinflammatory balance (or immunosignature) which you said was immunobabble. I brought it up because I think that some people (especially those on this forum) might actually be thinking of such a balance/signature when they talk about Th1/Th2. I cannot say for sure what Lipkins means by it, since as he doesn´t visit this forum I am not able to ask him.
Jonathan Edwards
"Gibberish"
- Messages
- 5,256
Well, I was just defending idea of a proinflammatory/antinflammatory balance (or immunosignature) which you said was immunobabble. I brought it up because I think that some people (especially those on this forum) might actually be thinking of such a balance/signature when they talk about Th1/Th2. I cannot say for sure what Lipkins means by it, since as he doesn´t visit this forum I am not able to ask him.
Yes I think the idea of balance is babble. If you have an up button on a lift and a down button, what is balance? Stuck on the third floor? It has no basis in serious systems dynamics. It was invented by people with tunnel vision.
Hip
Senior Member
- Messages
- 17,874
@msf, the Th1/Th2 balance idea does not refer to a pro-inflammatory / anti-inflammatory balance, but rather to the relative activations of two different branches of the immune response: the Th1 branch, which targets intracellular infections (such as viruses and intracellular bacteria like Chlamydia pneumoniae), and the Th2 branch, which targets extracellular infections like bacteria.
I understand that in mice, the Th1 and Th2 responses are quite mutually exclusive and polarized, so that when Th2 is engaged, it prevents the engagement of Th1, and vice versa. In other words, you cannot have both Th1 and Th2 at the same time.
This is how the idea of the Th1/Th2 balance came into being. The idea is that if the Th1 side of the seesaw is raised, then the Th2 side will be lowered. So the idea is that you cannot effectively fight both Th1 and Th2 infections at the same time, at least im mice.
But it turns out that in humans, the Th1 and Th2 responses are not as polarized and mutually exclusive as they are in mice, so the idea of seesaw balance does not apply as much to humans. Humans are more able to raise both sides of the seesaw at the same time.
The way that the Th1/Th2 balance has been applied to ME/CFS is as follows:
The chronic active infections linked to ME/CFS are intracellular infections, so the theory goes that you need the Th1 branch to fight these. The idea is that ME/CFS patients might be shifted towards Th2, thus preventing them from mounting a good Th1 response. But as I said, the Th1 and Th2 responses are not that polarized in humans, so the validity of the Th1/Th2 balance in ME/CFS needs to be questioned.
Certainly though enteroviral persistence is associated with ongoing ME/CFS, and enteroviral clearance or reduction in enteroviral loads is associated with remission or amelioration in ME/CFS symptoms. Dr Chia has found that with his oxymatrine, ribavirin and interferon treatments for ME/CFS, enteroviral loads went down as ME/CFS symptoms abated. And Dr Chia did show that enteroviral clearance from oxymatrine treatment was associated with an increase in the IL-12 / IL-10 ratio (these are Th1 and Th2 cytokines respectively), which implies an increase in the Th1/T2 ratio.
So although the validity of the Th1/Th2 balance in ME/CFS needs to be questioned, the general idea that there is something in ME/CFS patients' bodies or immune system that is preventing viral clearance still remains. If we can figure out what this assumed blocking factor is that prevents viral clearance, we may be able to find a cure for ME/CFS.
This assumed blocking factor is also relevant to chronic enteroviral myocarditis, where an acute enteroviral infection of the heart muscle does not resolve in some patients, but remains as a chronic persistent infection.
Over the years, I have been on the lookout for possible explanations of why an infection fails to resolve, and remains persistent.
I understand that in mice, the Th1 and Th2 responses are quite mutually exclusive and polarized, so that when Th2 is engaged, it prevents the engagement of Th1, and vice versa. In other words, you cannot have both Th1 and Th2 at the same time.
This is how the idea of the Th1/Th2 balance came into being. The idea is that if the Th1 side of the seesaw is raised, then the Th2 side will be lowered. So the idea is that you cannot effectively fight both Th1 and Th2 infections at the same time, at least im mice.
But it turns out that in humans, the Th1 and Th2 responses are not as polarized and mutually exclusive as they are in mice, so the idea of seesaw balance does not apply as much to humans. Humans are more able to raise both sides of the seesaw at the same time.
The way that the Th1/Th2 balance has been applied to ME/CFS is as follows:
The chronic active infections linked to ME/CFS are intracellular infections, so the theory goes that you need the Th1 branch to fight these. The idea is that ME/CFS patients might be shifted towards Th2, thus preventing them from mounting a good Th1 response. But as I said, the Th1 and Th2 responses are not that polarized in humans, so the validity of the Th1/Th2 balance in ME/CFS needs to be questioned.
Certainly though enteroviral persistence is associated with ongoing ME/CFS, and enteroviral clearance or reduction in enteroviral loads is associated with remission or amelioration in ME/CFS symptoms. Dr Chia has found that with his oxymatrine, ribavirin and interferon treatments for ME/CFS, enteroviral loads went down as ME/CFS symptoms abated. And Dr Chia did show that enteroviral clearance from oxymatrine treatment was associated with an increase in the IL-12 / IL-10 ratio (these are Th1 and Th2 cytokines respectively), which implies an increase in the Th1/T2 ratio.
So although the validity of the Th1/Th2 balance in ME/CFS needs to be questioned, the general idea that there is something in ME/CFS patients' bodies or immune system that is preventing viral clearance still remains. If we can figure out what this assumed blocking factor is that prevents viral clearance, we may be able to find a cure for ME/CFS.
This assumed blocking factor is also relevant to chronic enteroviral myocarditis, where an acute enteroviral infection of the heart muscle does not resolve in some patients, but remains as a chronic persistent infection.
Over the years, I have been on the lookout for possible explanations of why an infection fails to resolve, and remains persistent.
ljimbo423
Senior Member
- Messages
- 4,705
- Location
- United States, New Hampshire
The chronic active infections linked to ME/CFS are intracellular infections, so the theory goes that you need the Th1 branch to fight these. The idea is that ME/CFS patients might be shifted towards Th2, thus preventing them from mounting a good Th1 response. But as I said, the Th1 and Th2 responses are not that polarized in humans, so the validity of the Th1/Th2 balance in ME/CFS needs to be questioned.
I agree that the th1/th2 shift or teeter totter theory might not apply to cfs, although I thought it use to. I don't think there is a "shift" towards th2, so much as the th1 arm becomes exhausted over time, leaving a higher th2. I also wonder if the antiviral drugs, oxymatrine etc, are lowering viral levels.
Therefore giving the th1 arm of the immune system a chance to strengthen, leading to symptom improvement?
lansbergen
Senior Member
- Messages
- 2,512
The immune modulator I use shifts the response more towards Th1
ljimbo423
Senior Member
- Messages
- 4,705
- Location
- United States, New Hampshire
The immune modulator I use shifts the response more towards Th1
Have you noticed any symptom improvement?
lansbergen
Senior Member
- Messages
- 2,512
Have you noticed any symptom improvement?
I was dying and after I started taking the immunemodulator I very slowly imporved.
Many symptoms disappeared and others decreased. I am not cured but muxh better.
ljimbo423
Senior Member
- Messages
- 4,705
- Location
- United States, New Hampshire
I was dying and after I started taking the immunemodulator I very slowly imporved.
Many symptoms disappeared and others decreased. I am not cured but muxh better.
That sounds like a big improvement! Anything that gives a significant improvement is always welcome!
lansbergen
Senior Member
- Messages
- 2,512
That sounds like a big improvement! Anything that gives a significant improvement is always welcome!You must have been pleasantly surprised?
The surprise was that it eased the horrible pain enough to let me sleep a few hours. I still haven't seen a paper that mentions painrelief.
Hip
Senior Member
- Messages
- 17,874
th1 arm becomes exhausted over time, leaving a higher th2.
I have never come across a "Th1 exhaustion" hypothesis. Did you read about this somewhere?
However, there are several factors known to induce Th2 cytokines which might in theory inhibit a Th1 response.
And there is also the issues of immune evasion, which makes viral clearance difficult. For example, coxsackievirus B strongly inhibits antigen presentation by MHC class I, effectively making CVB-infected cells invisible to CD8 immune surveillance. All pathogens use immune evasion tricks like this to thwart the immune response.
Some viruses like EBV, cytomegalovirus and HHV-6 are cunning enough to make their own (fake) version of the human cytokine IL-10 (a Th2 cytokine) as part of their immune evasion strategy, which thwarts the antiviral immune response.
halcyon
Senior Member
- Messages
- 2,482
This is what happens in T cell exhaustion. As the cells become more and more downregulated, they stop producing th1 cytokines.I have never come across a "Th1 exhaustion" hypothesis. Did you read about this somewhere?
@msf, the Th1/Th2 balance idea does not refer to a pro-inflammatory / anti-inflammatory balance, but rather to the relative activations of two different branches of the immune response: the Th1 branch, which targets intracellular infections (such as viruses and intracellular bacteria like Chlamydia pneumoniae), and the Th2 branch, which targets extracellular infections like bacteria.
I understand that in mice, the Th1 and Th2 responses are quite mutually exclusive and polarized, so that when Th2 is engaged, it prevents the engagement of Th1, and vice versa. In other words, you cannot have both Th1 and Th2 at the same time.
This is how the idea of the Th1/Th2 balance came into being. The idea is that if the Th1 side of the seesaw is raised, then the Th2 side will be lowered. So the idea is that you cannot effectively fight both Th1 and Th2 infections at the same time, at least im mice.
But it turns out that in humans, the Th1 and Th2 responses are not as polarized and mutually exclusive as they are in mice, so the idea of seesaw balance does not apply as much to humans. Humans are more able to raise both sides of the seesaw at the same time.
The way that the Th1/Th2 balance has been applied to ME/CFS is as follows:
The chronic active infections linked to ME/CFS are intracellular infections, so the theory goes that you need the Th1 branch to fight these. The idea is that ME/CFS patients might be shifted towards Th2, thus preventing them from mounting a good Th1 response. But as I said, the Th1 and Th2 responses are not that polarized in humans, so the validity of the Th1/Th2 balance in ME/CFS needs to be questioned.
Certainly though enteroviral persistence is associated with ongoing ME/CFS, and enteroviral clearance or reduction in enteroviral loads is associated with remission or amelioration in ME/CFS symptoms. Dr Chia has found that with his oxymatrine, ribavirin and interferon treatments for ME/CFS, enteroviral loads went down as ME/CFS symptoms abated. And Dr Chia did show that enteroviral clearance from oxymatrine treatment was associated with an increase in the IL-12 / IL-10 ratio (these are Th1 and Th2 cytokines respectively), which implies an increase in the Th1/T2 ratio.
So although the validity of the Th1/Th2 balance in ME/CFS needs to be questioned, the general idea that there is something in ME/CFS patients' bodies or immune system that is preventing viral clearance still remains. If we can figure out what this assumed blocking factor is that prevents viral clearance, we may be able to find a cure for ME/CFS.
This assumed blocking factor is also relevant to chronic enteroviral myocarditis, where an acute enteroviral infection of the heart muscle does not resolve in some patients, but remains as a chronic persistent infection.
Over the years, I have been on the lookout for possible explanations of why an infection fails to resolve, and remains persistent.
Yes, I was aware of what Th1/Th2 theory actually entails. I wasn´t aware (until Snow Leopard posted the link) of the arguments against it. I however was suggesting that when some people say Th1/Th2 on this forum (or perhaps elsewhere too) they really mean something about proinflammatory/antinflammatory states. Perhaps this was ungrounded, but it was just a suggestion, and I would be surprised if everyone on PR had the same understanding of Th1/Th2, since we don´t see eye-to-eye on anything else!
Hip
Senior Member
- Messages
- 17,874
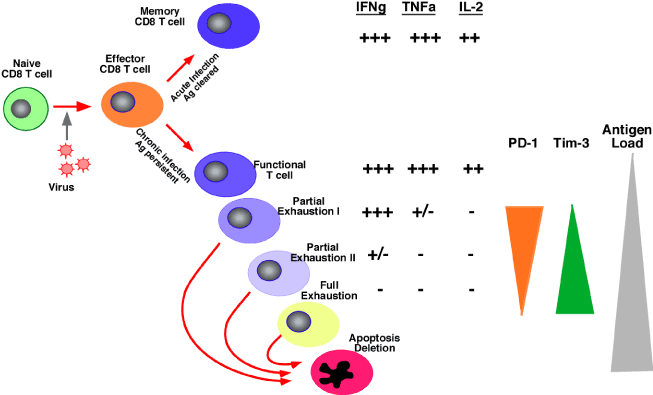
This is what happens in T cell exhaustion. As the cells become more and more downregulated, they stop producing th1 cytokines.
I don't remember coming across the concept of "T-cell exhaustion" before, so this is new concept for me. Is this what you were thinking about @ljimbo423 when you mentioned "Th1 exhaustion"?
This paper looks to be a good overview of T-cell exhaustion:
Highlights
- Persistent viral infections can result in the exhaustion of anti-viral T cells.
- Excessive and sustained levels of viral antigen drive T cell exhaustion.
- Exhausted T cells are distinct from typical effector and memory subsets.
- Exhausted T cells are functionally ineffective and compromise viral clearance.
- Blocking inhibitory receptors and modifying cytokine levels can alleviate exhaustion.
I wonder if there is any relation between CD8 T-cell exhaustion in chronic coxsackievirus B infection, and the fact that coxsackievirus B makes the cells it infects invisible to CD8 T-cells.
This paper claims to have found the cause of T-cell exhaustion during chronic viral infection: High antigen levels are the cause of T cell exhaustion during chronic viral infection.
And this paper claims to have found evidence for CD8 T-cell exhaustion in ME/CFS patients.